AbstractThe next generation of healthcare will be decentralized, mobilized, and personalized. Instead of the blunt instruments of the past, we will be giving patients more precise medications and therapies.Anita GoelChair and Scientific Director, Nanobiosym Research Institute
The paper sets out to examine the relevance of blockchain technology for healthcare management in general, and specifically for consumer medical electronics and connected portable devices. After considering the pivotal role of electronic health records in the first part of the paper, we then analyze the holistic transformative role of blockchain for healthcare data management, illustrated by a set of emerging use cases. Following that, we address the fast-growing segment of consumer medical electronics and the Internet of Medical Things. Finally, we highlight the digital community-building role of public private partnerships for emerging healthcare strategy design.
Introduction
Healthcare involves the preservation of health by safety, diagnosis, and disease and/or injury treatment. It encompasses several essential industries for the delivery of healthcare services and goods. Healthcare data is paramount insofar as it helps the healthcare system construct a detailed image analysis that examines the patient holistically, including their physical, mental, and emotional health, while taking into account social factors (Biswas & Muthukkumarasamy, 2017).
From a legislative and strategic standpoint, healthcare is one of the pillars of critical infrastructure in both the European NIS directive (European Parliament and the Council, 2016) and in the Health Insurance Portability and Accountability Act (HIPAA) security rule in the USA (Scholl et al., 2008). Healthcare is a priority for the European Commission (2020a, 2020b) that advocates an artificial intelligence-based approach, along with the creation of a common European health data space, to help authorities make evidence-based decisions (Naqvi & Hussain, 2020). Manion and Bizouati-Kennedy (2020) found that global expenditure on research and development across all industries amounts to $1.7 trillion annually out of which more than $300 billion is spent on medical research. In this article, we assess the following research question: does the plurality of organizational and institutional arrangements and healthcare data vehicles shed new light on blockchain-powered Electronic Health Records (hereafter EHRs), thereby enabling a deeper patient-centric turn in healthcare management?
After a short methodology section, the paper analyses the transformative role of blockchain for the management of EHRs in the second section. After exploring the role of evoking public-private partnerships for innovative healthcare blockchain design, it then addresses the fast-growing segment of consumer medical electronics and the Internet of Medical Things.
Methodology and Structure
Section 2 examines EHRs, which constitute health data management enablers, both through online and offline solutions, such as with data lakes. Further, I examine use cases, and showcase that despite the diversity of organizational forms and underlying healthcare data vehicles, the former converge toward a patient-centric approach. Section 3 takes a systemic height to analyse the holistic transformative power of blockchain technology on the healthcare sector. Section 4 discusses the multiplicity of objectives and organizational forms featuring some concrete and current large-scale projects.
Electronic Health Records (EHRs) and Blockchain Technology
What are EHRs, and why does their management matter?
Research on enhanced medical information systems among clinics and hospitals dates back to the 1960s (Kim et al. 2019, Bittins et al., 2021). Today, in a globalized world marked by mobility, patient data is scattered and fragmented along institutional and national lines and circumscribed into data silos that are more easily accessible to the healthcare provider than the patient (Reisman, 2017). EHRs consist of a patient's medical records in digital format, comprising clinical data stored with a specific care provider, including Magnetic resonance imaging (MRI) reports, past medical examinations, immunizations, laboratory reports, a list of allergies, etc. (Kumaraswamy & Manhar, 2020). The maintenance and updating of EHRs does not always go without problems. The broad issue of data sharing and coordination is called interoperability (Office of the National Coordinator for Health Information Technology, 2015). In a US survey of Health Exchange Information (HIE) leaders, 50% of respondents reported that EHR vendors routinely engage in information-blocking practices, either by designing products with limited interoperability, or charging high fees for providing HIE capabilities (Adler‐Milstein & Pfeifer, 2017). Write and read permissions ought to be thoroughly managed, as not all health records can or should be made available to patients (U.S. Department of Health & Human Services, 2017). As we will see later in the paper, blockchain technology precisely allows this type of real-time tamperproof monitoring, as well as providing an entryway into interoperability (Goldwater, 2016).
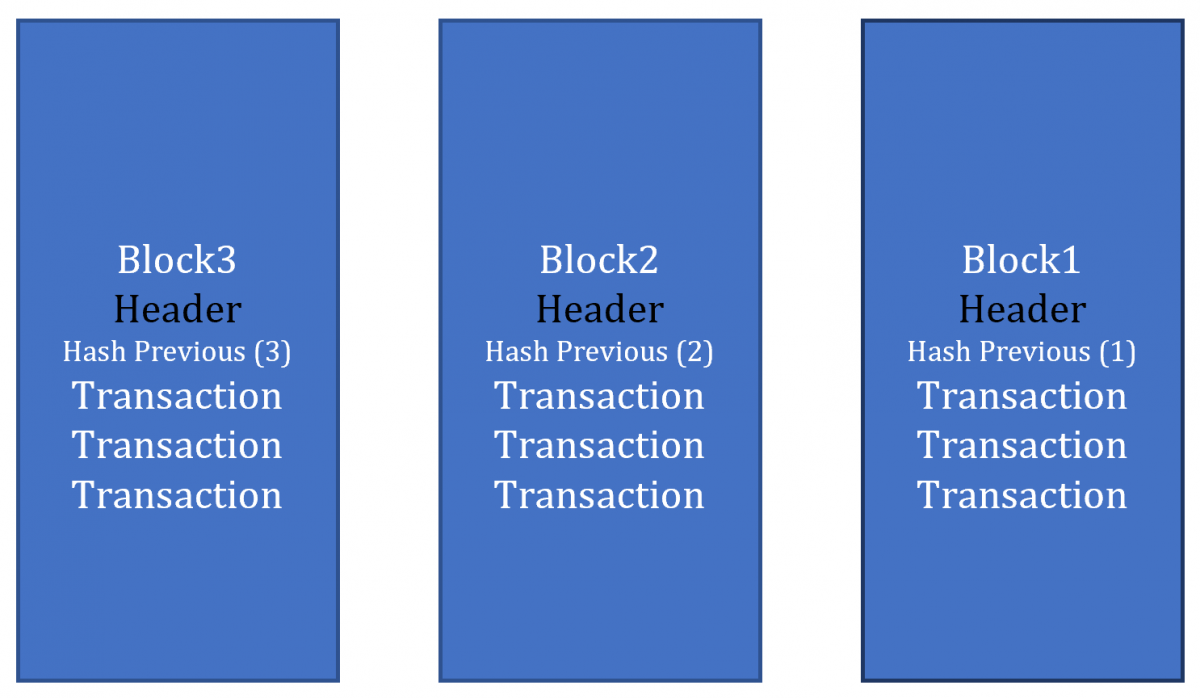
Figure 1. Blocks and groups of transactions
The Indian web and mobile app development company BR SofTech (www.brsoftech.com) forecasts the blockchain healthcare market to be worth $829 Million by 2023. A blockchain-driven health information exchange (BHIE) unlocks the value of interoperability and cybersecurity, with the potential to eliminate frictions and costs of existing third-party intermediaries, improve data integrity, and reduce transaction costs. The coordination of patientcare by some kind of BHIE would alleviate unnecessary services and duplicate tests, even while coming with lower costs and enhanced efficiencies of the continuum care cycle.
An important innovation in the management of EHRs is MedRec, which provides open record-keeping, authorization, and data sharing among healthcare stakeholders. The platform “gives patients a comprehensive, immutable log and easy access to their medical information across providers and treatment sites”. MedRec draws on blockchain technology to ensure authentication, confidentiality, accountability, and data sharing (Azaria et al., 2016).
The solution incentivizes actors in medical communities to participate in blockchain-enabled digital ecosystems. The advantages of BHIEs are substantial. MedRec enables faster access to medical data, improves system operability, solves issues of patient agency (that is, full information to the patients about their medical history and any modifications to it), and finally improves the quality/quantity of data available for medical research purposes (Azaria et al., 2016).
Noteworthy, is that it is not EHRs themselves that are stored on a blockchain distributed ledger, but rather the digital signature thereof, grouped in an index akin to a library card catalog. For the patient, the benefits are invaluable. They are constantly informed about the read- and write-permissions concerning EHRs, and where the latter can be sent (Halmanka et al., 2017). A trade-off exists in healthcare technological solutions between care and privacy, on the hand one, and economic fraud for patients on the other hand. This is an issue being exacerbated by the expanding mass of data continuously generated by the healthcare system. Nevertheless, it has been noted that, “[b]lockchain's secure technology, properties, and distributed nature can help reduce the cost and efficiency of these operations as well as provide a viable security infrastructure” (McFarlane et al., 2017). The siloed and fractured nature of current billing and payment systems for both private and public health systems also reinforces the risk of fraud (Manion & Bizouati-Kennedy, 2020). For instance, Change Healthcare is a large health coverage organization in the USA, which has adopted blockchain for the purpose of billing and payments. They made a strategic acquisition in 2018 with PokiDok1, a pioneer in blockchain-based healthcare solutions.
Offline and off-chain data containers: data lakes
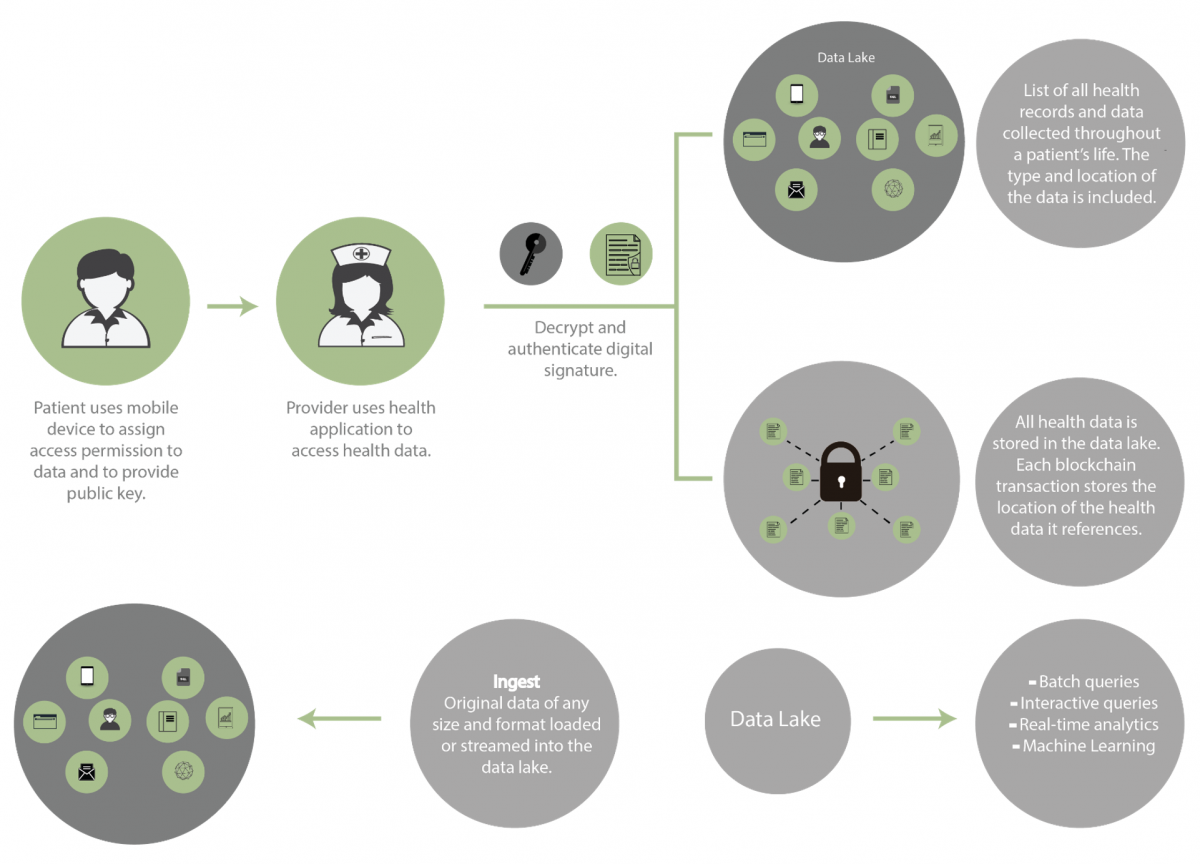
Linn and Koo (2016) proposed a similar blockchain-based solution, focusing on offline and off-chain data containment, so-called data lakes. A health-oriented blockchain would contain a complete indexed history of all available medical data, including formal medical records as well as health data from mobile applications and wearable sensors, and would follow an individual user throughout their life. All medical data would be stored off blockchain in a data repository called a data lake. Data lakes are highly scalable and can store a wide variety of data, from images to documents to key value stores.
The increasingly popular data lakes (Rangarajan et al., 2015) rely on a flat architecture to store data in their raw format (Immon, 2016). Data lakes store huge quantities and wide varieties of encrypted and digitally signed medical data, thereby ensuring privacy and authenticity of the healthcare information. Each data entity is associated with a unique identifier and a set of extended metadata. One can use purpose-built schemas for query-relevant data resulting in a smaller set of data for the purpose of answering a given question. A metadata repository that registers high-level information about data entities is paramount in the data lake structure. Serious concerns persist regarding the fuzziness and even the incomprehensibility of healthcare data, due to the lack of an appropriate interpretative grid, which thereby turns a data lake into a data swamp (Hai et al., 2016). Combined with machine learning tools, these data lakes greatly simplify interactive queries and real-time big data analytics (Linn & Koo, 2016).
Figure 2. Data lakes
Source: Adapted from Linn & Koo (2016)
Linn and Koo (2016) stressed the role of open APIs used to integrate and exchange data with various blockchains. They emphasized the great variety of information sources that may be used by the new digital ecosystems (blockchain + offline data lakes), such as mobile applications and consumer medical electronics (Internet of Medical Things).
Use Cases with Electronic Health Records and consumer wearables
The Mayo Clinic (Peterson et al., 2016) investigated data sharing and interoperability in healthcare by designing a new algorithm. The study’s authors addressed the security issue with the help of network-wide keys and smart contracts. CEO of Humana, Bruce Broussard (2016) thinks that blockchain technology and smart contracts will become pivotal in the healthcare industry through the automatic verification and authorization of information related to payments and payer contracts, which will be conducive to efficiency gains.
Gem Health was launched in 2016. It aims at developing blockchain applications and shared infrastructure for healthcare that solve important issues of digital identity and interoperability (Vergel de Dios, 2016). To address operating costs, the Gem Health Network2 powered by Ethereum, was launched by Gem in collaboration with Philips Blockchain Lab (Shen et al. 2019).
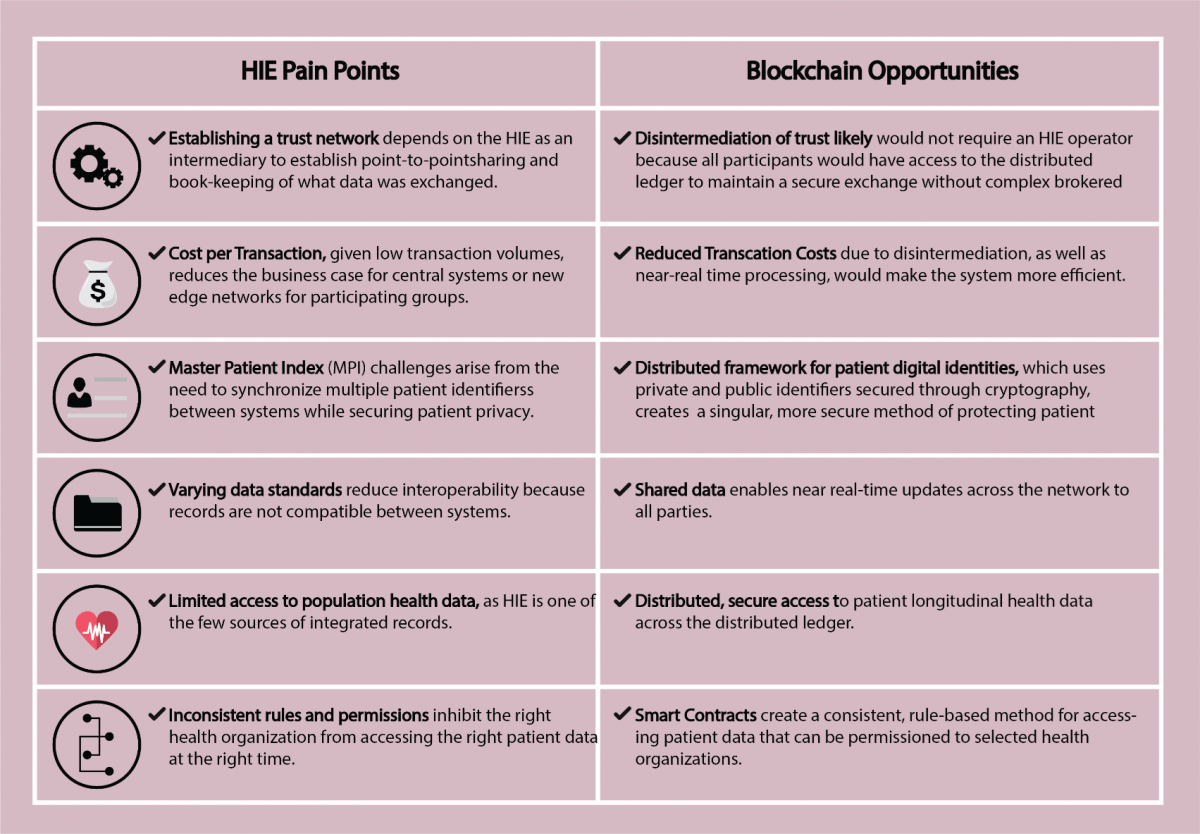
Figure 3. HIE pain points and blockchain opportunities,
Adapted from Deloitte (2016)
A promising initiative comes from Deloitte Netherlands in collaboration with SNS Bank and Radbou, who have developed Prescrypt (Justinia, 2019), a proof-of-concept that helps verify a patient’s digital identity, genetics data, or prescription history, by giving patients full ownership of their medical records, thereby allowing them to grant and revoke provider access to their data (Deloitte, 2016).
A veritable revolution is underway in patientcare driven by the growth in wearables and consumer medical electronics. Whereas consumer medical electronics are a high-growth segment at the intersection between medical electronics (see figure 5) and consumer electronics, wearables are “devices that can be worn or mated with human skin to continuously and closely monitor an individual's activities, without interrupting or limiting the user's motions” (Gao et al, 2016).
Drawing on osteoarthritis, Papi et al. (2015) showed that the quality of medical data generated by wearables provided medical information to practitioners on par with other research methods and tools, such as surveys. Goldwater (2016) stated that “patient-related outcome measures (PROMs), which focus on outcomes that are directly related to the patient, have taken on added importance and significance over the past several years”. Healthcare services are shifting from a centralized, hospital-oriented model toward a distributed patient-centric model relevant for future blockchain applications.
We distinguish between (1) medical imaging, (2) consumer and portable medical, (3) medical instruments and diagnostics, and (4) patient monitoring and therapy. We focus in this section on the first category that now intersects with IoMT (Internet of Medical Things). An alternative to the use of standardized instruments to collect data and provide a foundation for the development of PROMs is the use of IoMT. The latter addresses the problem of storing personal health data gathered from consumer medical devices and software such as wearables and mobile on the cloud. Notwithstanding, PROMs are not short of pitfalls. Frost et al. (2007) showed that the objective and accurate measurement (that is, psychometrically validated) of a patient’s feelings is a complex and costly technological endeavor.
The IoT cannot be the panacea to all the barriers to PROM development and use, but the information generated from wearables, smartphone applications and other patient-centered technology, can provide a basis for understanding what types of measures can and should be developed (Goldwater, 2016).
While the IoT, often heralded as a revolution (Evans, 2011), refers to connected objects through a network-based concept that functions with the help of sensors, electronics, and software applications, the IoMT refers to self-tracking devices and personal environment monitoring applications (for example, digital health monitoring automation, ambient behavior management suggestions and other real-time personalized recommendations) (Goldwater, 2016). Typical examples are consumer medical wearables and sensors that keep track of changes in pressure, temperature, motion, light, and sound, which are particularly adapted to the present needs of the healthcare industry.
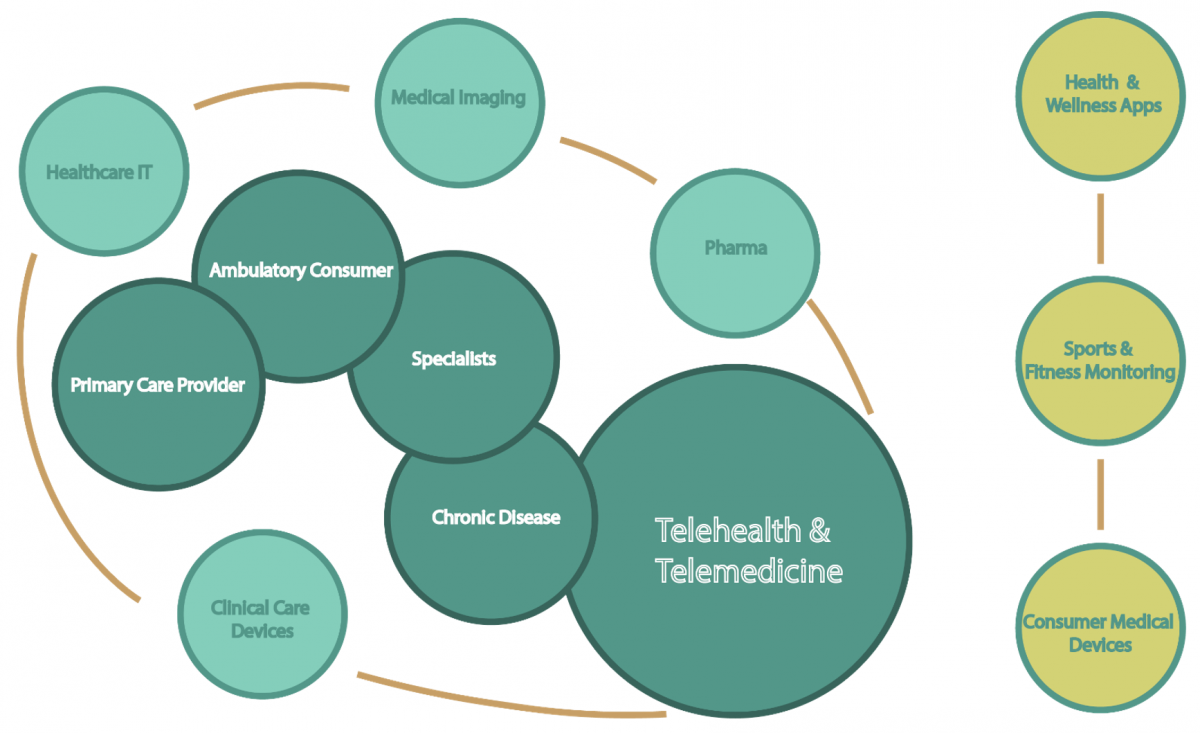
Figure 4. Major players in the health devices/apps market
Adapted from Bodenheimer (2017)
PROMs include quality-of-life indicators such as physical and social functions, treatment adherence, and satisfaction with treatment. They improve the accuracy of patient-physician communication in terms of the burden of treatment-related morbidities by providing a more detailed and complete evaluation of treatments for specific conditions, such as cancer or multiple sclerosis (Valderas et al., 2008). Personal health devices are generally characterized by miniaturization, portability, wireless functionality, and customization. The ingredients of success are ultra-low power consumption, battery life, reduced size and cost, and the existence of microcontrollers. Wearables and sensors are “always-on”, thereby medical information is being generated around the clock.
Furthermore, blockchain technology gives the patient control over the types of data released. Recent developments, such as Google Fit (2020) and Apple Health Kit (2020), have move towards re-integrating the patient into established data exchanges (Bittins et al., 2021). Through the tree structure of the protocol, the provider validates the information as coming from the patient upon reception. Data provenance determination, a key generic blockchain use case, is carried out through a unique digital signature. Full control is retained by the protocol regarding the entities that can access the data; and what specific elements thereof can be used. A fundamental application is self-sovereign identity management that securely controls identity claims over a range of health authorities at various jurisdictional levels (Mühle et al., 2018; Tobin & Reed, 2018).
Market drivers include an aging population, rising healthcare costs, new lifestyle diseases (for example, obesity), growing awareness amongst consumers (for example, preventive health and wellness management), and a shortage of trained medical staff (Srinivasa, 2011; Frost & Sullivan, 2012). Key market players include Devices, Inc., Cypress Semiconductor Corporation, Fairchild Semiconductor International, Inc., GE Healthcare Pvt. Ltd, Maxim Integrated Products, Inc., NXP Semiconductors N.V., On Semiconductor Corporation, Philips Healthcare Pvt. Ltd., Renesas Electronics Corporation, Siemens Ag, STMicroelectronics N.V., Tekscan, Inc., and Texas Instruments, Inc. A.
IoMT facilitates the measurement of critical elements such as vital signs (Peng et al., 2012), electrocardiogram (ECG) and electroencephalogram (EEG) measurement, skin temperature, etc. IoMT allows people to monitor health parameters, such as body weight, heart rates, burned calories, sleep patterns, blood sugar levels, and a variety of fitness-related metrics, as well as monitoring of nutrition and medication intake (Bodenheimer, 2017) with new opportunities such as “more collaborative patient engagement, reconciliation of data across different silos, health information sharing, and quality data reporting” (Ibid). This helps to shape the health care system so that patients “create and manage their different providers and family members”, and “caregivers view, edit, and share an integrated and centralized personal health record” (Ibid). Goldwater (2016) saw numerous possibilities through the pairing of blockchain with smartphone applications, such as Lantern, Optimism, and Medisafe.
Figure 5. Health IT ecosystem in 2040
Adapted from: IHS, 2015
Figure 6 forecasts the Health IT ecosystem in 2040. However, to be complete, key areas, such as genomics, DNA sequencing, and health blockchain apps are arguably missing (Stanganelli, 2016; Brennan, 2017; Lin 2017). As Stanganelli (2016) argued, “[t]he inherent provenance benefits of blockchain are allowing the healthcare and life-science industries to indelibly record medicinal and genomic data that will effectively combat counterfeit pharmaceuticals and protect intellectual property”.
Blockchain: a decentralized solution for healthcare management?
Blockchain is the technology behind the Bitcoin protocol, and is traced to the pseudonymous, unidentified person (or group) known as Satoshi Nakamoto (2008). It consists of a data structure that creates trusted, distributed digital ledgers for assets and other data. It is an immutable record of digital events shared peer-to-peer between different parties. It can only be updated by a consensus majority of the participants in the system and, once entered, the ledger is quasi-immutable (Frost & Sullivan, 2019).
A blockchain ledger is a digital system for executing and recording timestamped transactions (and by extension and type of collected data), grouped in so-called “blocks”. Each block contains a hash of the previous block, transaction data, and the hash of this block. Blockchain ledgers draw on intelligent algorithms, and are secured by means of cryptographic techniques (Pilkington, 2016).
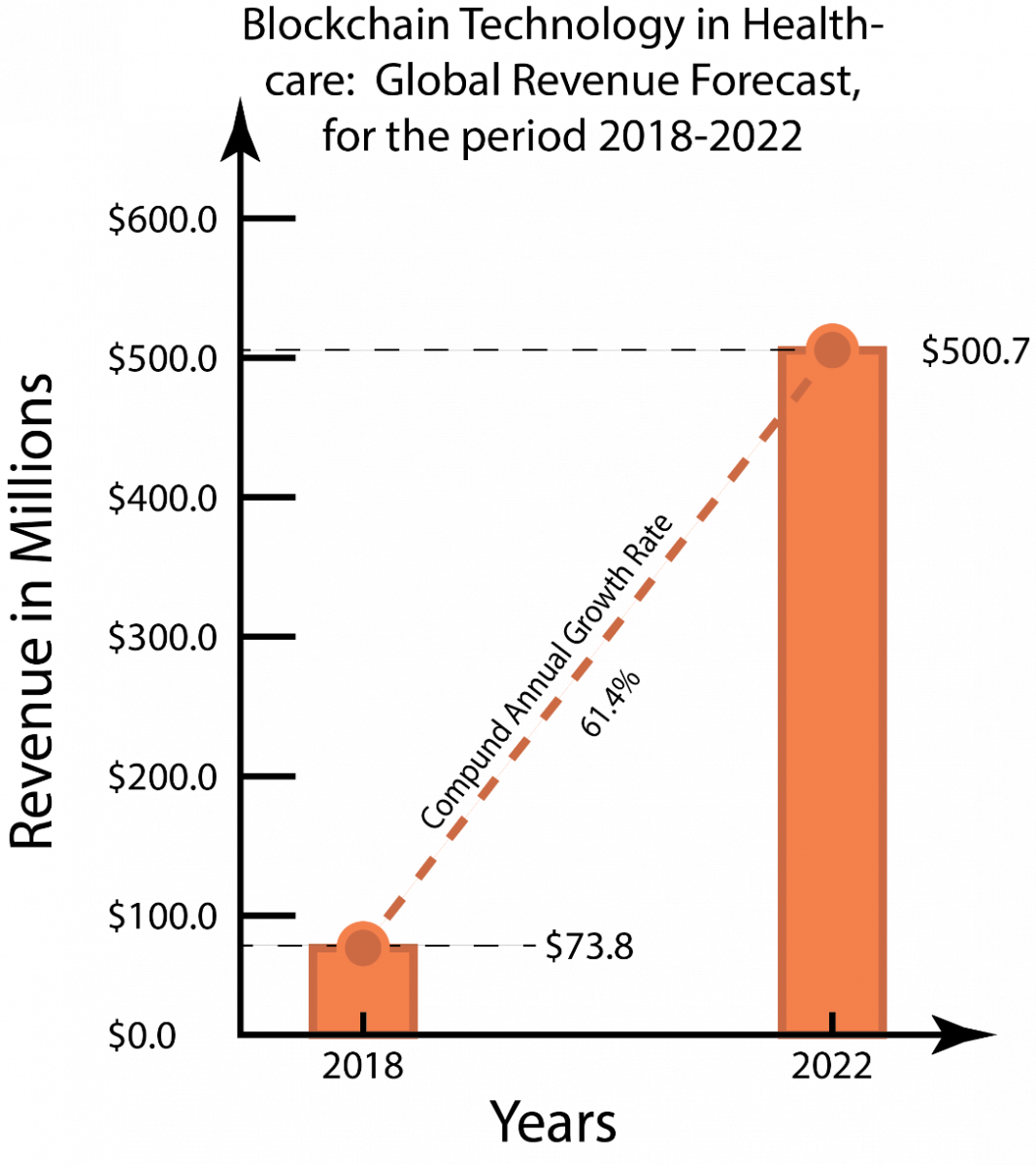
For Dr. Alex Cahana, ConsenSys Health Chief Medical Officer (cited by Manion & Bizouati-Kennedy, 2020), “blockchain is the solution to the social issue of trust. We live in a world where I want to trust everything, but I just can’t”. As per the reports of Statista (Statista, n.d.), the worldwide market of Blockchain is 3.9 billion USD in 2020 and expecting to grow to 23.3 billion USD by 2023. Blockchain technology has become a novel decentralized solution for enhanced healthcare information management. Deloitte (2016) listed blockchain opportunities in the healthcare sector, as presented in Figure 4. From disintermediation of trust, reduced transaction costs, digital identity management, shared data with secured access to patient longitudinal health data and smart contracts for accessing patient health data, blockchain technology holds a promise to transform the landscape of health care system management. Likewise, drawing on Justinia (2019), Kuo et al. (2017), and Frost and Sullivan (2019), Table 1, 2, and 3 present the advantages of blockchain technology for the healthcare sector. Figure 5 presents a 2018-2022 overview of the healthcare blockchain industry segment.
Figure 6. Revenue forecast (2018-2022)
Adapted from Frost & Sullivan (2019)
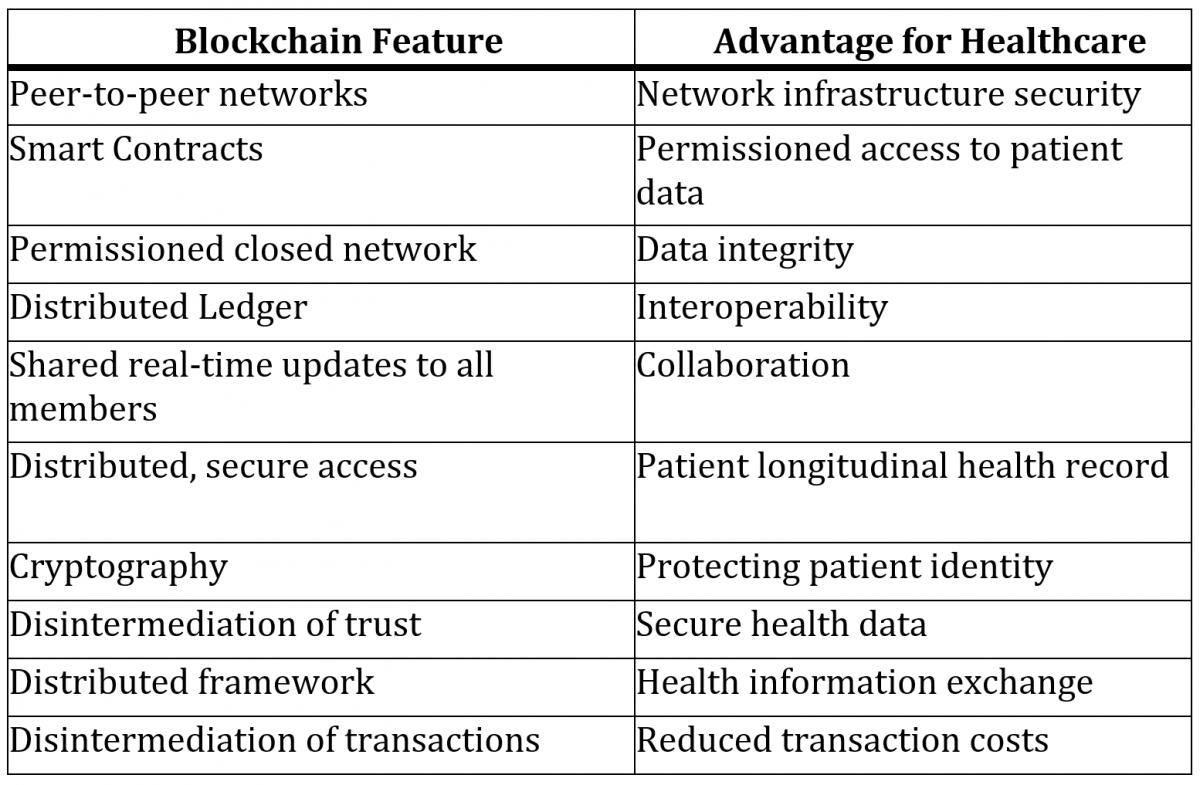
Table 1. Blockchain Advantages for Healthcare
Source: Justinia (2019)
Table 2. Blockchain benefits and use cases to advance biomedical/health care data ledger
Source : Kuo et al. (2017)
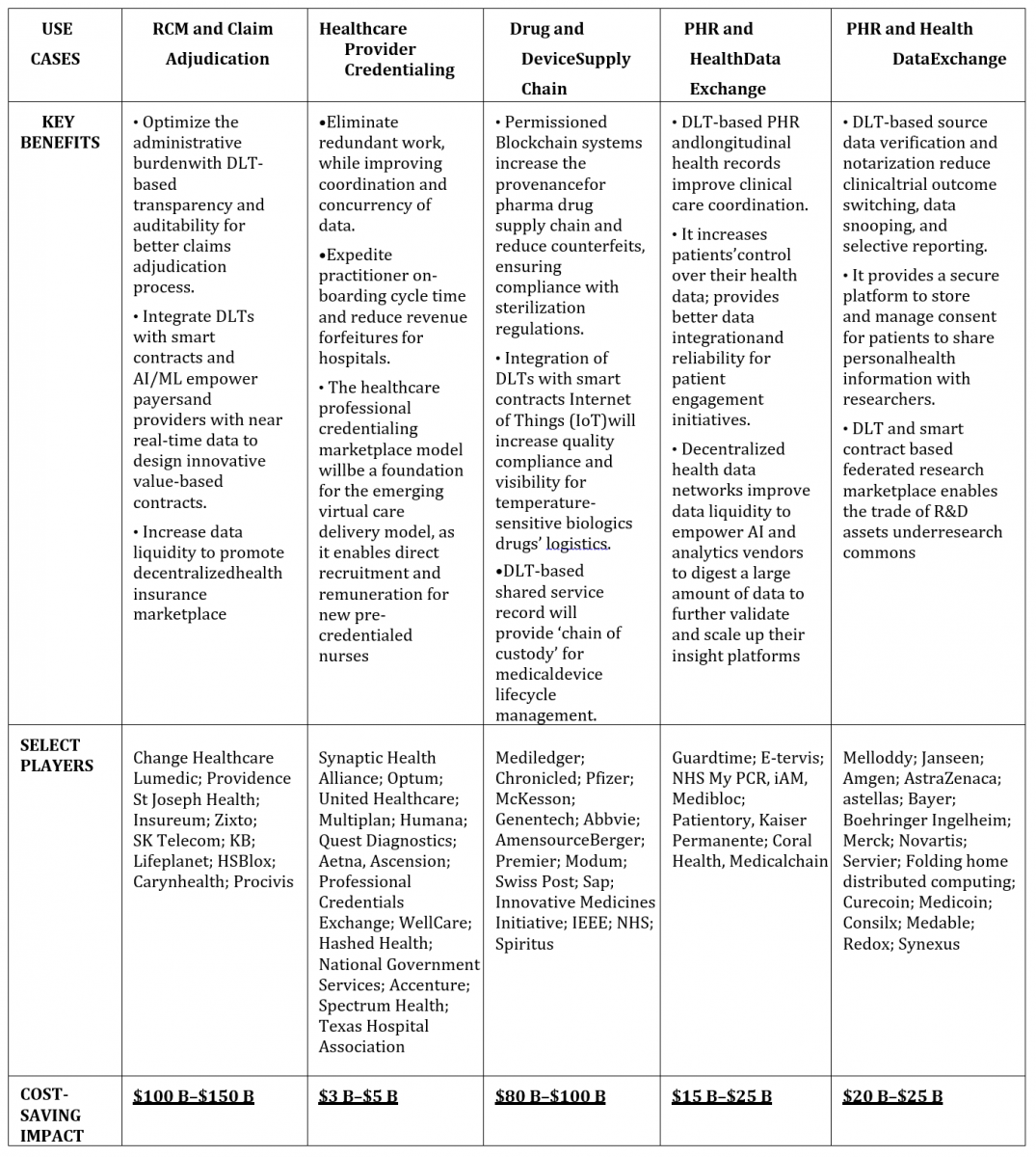
Table 3. Top 5 Growth Opportunities and Main Players by Use Case
Source: Frost and Sullivan (2019)
The IBM Institute for Business Value (2017) singled out the most disruptive effect that blockchain technology will have on healthcare systems, namely the creation of a common database that can be accessed from any electronic medical system. This would entail the elimination of trusted third parties and its corollary, a single point of failure (The Economist, 2015). Engelhardt (2017) identified four major advances enabled by blockchain: (1) patient-centric care, (2) privacy and access, (3) completeness of information, and (4) lower costs. Stagnaro (2019) listed five innovative use cases: longitudinal healthcare records, automated health claims adjudication, interoperability, online patient access, and supply chain management. Amongst all healthcare stakeholders, health insurance payers, providers, and pharma companies are expected to be the early adopters of blockchain systems, moving beyond pilot projects as early as 2021 into concrete blockchain-powered business-to-business (B2B) enterprise applications and creating much needed network effects in the healthcare space (Frost & Sullivan, 2019).
Discussion
A public private partnership (PPP) is a form of long-term contract, where a public entity transfers the provision of public health services to a private party. PPPs create opportunities for both the public and private partners to maximize each other’s strengths. The United Nations Sustainable Development Goal (SDG) number 17 sets out to encourage partnerships between governments, the private sector, and civil society to achieve the UN 2030 Development Agenda. PPPHealth4All is a knowledge platform that facilitates the preparation and implementation of people-centered PPP healthcare projects. At least 400 million people worldwide have no access to healthcare, there is a 31-year gap between countries with the shortest and longest life expectancies, and 5 million people die every year because of poor-quality health care in low- and middle-income countries (SDG.17 Consulting GmbH, 2021).
Emerging blockchain strategies have been deployed in the USA thanks to a recent piece of legislation (del Castillo, 2017) called the America Competes Reauthorization Act (US Congress, 2015-2016). The pharmaceutical industry has been an early adopter of blockchain technology.
The complexity and multi-stakeholder level conditions of drug supply chain management necessitates the setting up of consortia with representative parties that agree on consensus mechanism rules (Frost & Sullivan, 2019). Greatly enhanced by digitization (Bughin et al. 2017; Schrauf, 2017), new challenges are arising with globalization due to unprecedented network-driven complexity and prevailing geopolitical, technological, economic, and sanitary uncertainty (Chang et al, 2020; Ahir et al, 2021).
Blockchain can help the pharmaceutical industry better manage its transactions and improve record keeping across the whole supply chain. This will help combat counterfeit drugs and make compliance and traceability more efficient. The key property that blockchain has is that any information recorded on-chain is immutable. As blockchain is built on a distributed network and serving as an open ledger, the industry can trace a product through the whole supply chain and lifecycle (Curran, 2020).
The paper briefly presents hereafter two successful blockchain PPPs in the pharmaceutical industry.
The IEEE Pharma Blockchain Initiative
In November 2017, IEEE launched the Pharma Blockchain Initiative to evaluate DLTs for securing and optimizing the pharmaceutical supply chain. Palombani (2017) explains that the deployment of blockchain in the pharmaceutical supply chain needs to tackle the massive global counterfeit drug problem, beyond mere compliance matters, along with the societal cost of counterfeit drugs.
IMI Pharma Blockchain Consortium
The Innovative Medicines Initiative (IMI) aims to accelerate the development of and access to innovative medicines, particularly in underprivileged areas. It is based on a multi-stakeholder governance model that includes universities, research centers, the pharmaceutical industry and other industries, small and medium-sized enterprises (SMEs), patient organizations, and healthcare regulators. Signed between the EU and the European pharmaceutical industry, IMI is the world's biggest PPP in life sciences. IMI plans to develop next generation vaccines, medicines, and antibiotic treatments in the context of an aging population. IMI pharma blockchain consortium was designed to help members evaluate, design, and accelerate the adoption of distributed ledger technology across the drug supply chain and clinical trials.
Conclusion
Blockchain has the tremendous potential to open doors for enhanced interoperability, and allow for more performant, better managed, and easily transferable EHRs across data silos, institutional boundaries, and even national jurisdictions. Blockchain technology might become both the push and the pull factor of the health industry as regards data standardization, the former by means of cost-saving incentives, and the latter by providing a true value proposition thanks to the new standards in place (Manion & Bizouati-Kennedy, 2020). Standardized data provide a secure, transparent, and rapid system of tracking data, variables, and research that enhances the economic value extracted from data. The booming market for consumer medical electronics and the advent of the Internet of Medical Things (IoMT) are a testimony of the current transformation underway in the healthcare system toward self-managed and patient-centric models, which form an experimental field for emerging health applications.
References
Adler‐Milstein, J., & Pfeifer, E. 2017. Information Blocking: is it occurring and what policy strategies can address it? The Milbank Quarterly, 95(1): 117-135. Available online at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5339397/
Ahir, H., Bloom, N., & Furceri, D. 2021. From COVID-19 to Brexit, this is how Uncertainty Affects the Global Economy, World Economic Forum. Available online at: https://www.weforum.org/agenda/2021/01/global-uncertainty-index-economics-us-uk-covid-coronavirus-pandemic-brexit-china/
Apple Health Kit. 2020. Apple. Available online at: https://developer.apple.com/health-fitness/
Azaria, A., Ekblaw, T.V., & A. Lippman 2016. MedRec: Using Blockchain for Medical Data Access and Permission Management, 2016 2nd International Conference on Open and Big Data (OBD): 25-30. DOI: 10.1109/OBD.2016.11
Bittins, S., Kober, G., Margheri, A., Masi, M., Miladi, A., & Sassone, V. 2021. Healthcare Data Management by Using Blockchain Technology. In Applications of Blockchain in Healthcare: 1-27. Springer, Singapore. DOI: https://doi.org/10.1007/978-981-15-9547-9_1
Bodenheimer, L. 2017. IoT and Blockchain – Prescription for healthcare sector, Detecon Consulting. Available online at: http://www.deteconusa.com/iot-blockchain-healthcare-sector/
Brennan, B. 2017. Using Blockchain in Genomics. Blockchain Healthcare Review, Available online at: http://blockchainhealthcarereview.com/using-blockchain-in-genomics/
Broussard, B. 2017. Blockchain: Transformational Technology for Health Care, LinkedIn Post. Available online at: https://www.linkedin.com/pulse/blockchain-transformational-technology-health-care-bruce-broussard?trk=vsrp_people_res_infl_post_title
Bughin, J., LaBerge, L., &Melibye, A. 2017. The Case for Digital Reinvention. McKinsey Quarterly. February.
Chang, Y., Iakovou, E., & Shi, W. 2020. Blockchain in Global Supply Chains and Cross Border Trade: a critical synthesis of the state-of-the-art, challenges and opportunities. International Journal of Production Research, 58(7): 2082-2099.
Curran, K. 2020. Transforming Industry and Society: blockchain beyond the coin, Information Age. Available online at: https://www.information-age.com/transforming-industry-society-blockchain-beyond-coin-123490494/
del Castillo, M. 2017. Why the US Department of Health Just Couldn't Ignore Blockchain. Coindesk. Available online at: https://www.coindesk.com/why-the-us-department-of-health-just-couldnt-ignore-blockchain/
Engelhardt, M.A. 2017. Hitching Healthcare to the Chain: An Introduction to Blockchain Technology in the Healthcare Sector. Technology Innovation Management Review, 7(10). DOI: https://doi.org/10.22215/timreview/1111
European Commission. 2020. Communication from the Commission to the European Parliament, the Council, the European Economic and Social Committee, and the Committee of the Regions - a European strategy for data. Available online at: https://ec.europa.eu/info/sites/info/files/communication-annex-farm-fork...
European Commission. 2020. White Paper on Artificial Intelligence - A European approach to excellence and trust. Available online at: https://ec.europa.eu/info/publications/white-paper-artificial-intelligen...
European Parliament and the Council. 2016. Directive (EU) 2016/1148 of the 6th July 2016 Concerning Measures for a High Common Level of Security of Network and Information Systems Across the Union. Available online at: http://data.europa.eu/eli/dir/2016/1148/oj
Evans, D. 2011. The Internet of Things: how the next evolution of the Internet is changing everything [Internet] San Jose (CA). Cisco Internet Business Solutions Group. Available online at: http://www.cisco.com/c/dam/en_us/about/ac79/docs/innov/IoT_IBSG_0411FINAL.pdf.
Frost, M., Reeve, B., & Liepa, A. 2007. What is Sufficient Evidence for the Reliability and Validity of Patient-Reported Outcome Measures. Value In Health, 10(7): 94-105. DOI: https://doi.org/10.1111/j.1524-4733.2007.00272.x
Frost & Sullivan. 2012. Consumer Medical Electronics: A High Growth Segment for Semiconductors. Available online at : http://www.frost.com/sublib/display-market-insight.do?id=255626776
Frost & Sullivan. 2019. Global Blockchain Technology Market in the Healthcare Industry, 2018-2022, Healthcare Industry Assesses Blockchain Potential to Optimize Healthcare Workflows and Improve Outcome-based Care Delivery Models, Global Transformational Health Research Team. Available online at: https://store.frost.com/global-blockchain-technology-market-in-the-healthcare-industry-2018-2022.html
Gao, W., Emaminejad, S., Nyein, H.Y., Challa, S., Chen, K., Peck, A., et al. 2016. Fully Integrated Wearable Sensor Arrays for Multiplexed in Situ Perspiration Analysis. Nature; 529(7587): 509-514. DOI: https://doi.org/10.1038/nature16521
Goldwater, J.C. 2016. The Use of a Blockchain to Foster the Development of Patient-Reported Outcome Measures. Available online at: https://www.healthit.gov/sites/default/files/6-42-use_of_blockchain_to_develop_proms.pdf. Accessed 14 February 2021
Google Fit. 2020. Google. https://www.google.com/fit/.
Hai, R., Geisler, S., & Quix, C. 2016. Constance: An intelligent data lake system. In: Proceedings of the 2016 International Conference on Management of Data. SIGMOD’16, New York, NY, USA, ACM: 2097-2100. DOI: https://doi.org/10.1145/2882903.2899389
Halamka, D.M.D., Lippman, A., & Ekblaw, A. 2017. The Potential for Blockchain to Transform Electronic Health Records, Harvard Business Review. Available online at: https://hbr.org/2017/03/the-potential-for-blockchain-to-transform-electronic-health-records
IBM Institute for Business Value. 2017. Healthcare Rallies for Blockchains: Keeping patients at the center. The Economist Intelligence Unit. Available online at: https://www.ibm.com/downloads/cas/BBRQK3WY
Inmon, B. 2016. Data Lake Architecture: Designing the Data Lake and Avoiding the Garbage Dump. Technics Publications.
Justinia, T. 2019. Blockchain Technologies: Opportunities for Solving Real-World Problems. In Healthcare and Biomedical Sciences. Acta Informatica Medica, 27(4): 284. DOI: https://doi.org/10.5455/aim.2019.27.284-291
Kim, E., Rubinstein, S.M., Nead, K.T., Wojcieszynski, A.P., Gabriel, P.E., & Warner, J.L. 2019. The Evolving Use of Electronic Health Records (EHR) for Research. Seminars in Radiation Oncology, 29(4): 354-361. DOI: https://doi.org/10.1016/j.semradonc.2019.05.010
Kumaraswamy, R., & Manhar, A. 2020. Blockchain Technology in Healthcare Industry. International Journal of Scientific Research in Computer Science, Engineering and Information Technology, 6(6): 236-240. DOI: https://doi.org/10.32628/cseit206645
Kuo, T.T., Kim, H.E., & Ohno-Machado, L. 2017. Blockchain Distributed Ledger Technologies for Biomedical and Health Care Applications. Journal of the American Medical Informatics
Association, 24(6): 1211-1220. DOI: https://doi.org/10.1093/jamia/ocx068
Lin, P. 2017. Blockchain: The Missing Link Between Genomics and Privacy? Forbes. Available online at: https://www.forbes.com/sites/patricklin/2017/05/08/blockchain-the-missing-link-between-genomics-and-privacy/#6c2c74e64b77
Linn, L.A., & Koo, M.B. 2016. Blockchain for Health Data and its Potential Use in Health IT and Health Care Related Research. Available onlineat: https://www.healthit.gov/sites/default/files/11-74-ablockchainforhealthcare.pdf
Manion, S.T., & Bizouati-Kennedy, Y. 2020. Blockchain for Medical Research: accelerating trust in healthcare. CRC Press. DOI: https://doi.org/10.4324/9780429327735
McFarlane, C., Beer, M., Brown, J., & Prendergast, N. 2017. Patientory: A Healthcare Peer-to-Peer EMR Storage Network, 1(1). Available online at: https://patientory.com/patientory_whitepaper.pdf
Mühle, A., Grüner, A., Gayvoronskaya, T., & Meinel, C. 2018. A Survey on Essential Components of a Self-Sovereign Identity. Computer Science Review, 30: 80-86. DOI: https://doi.org/10.1016/j.cosrev.2018.10.002
Nakamoto, S. 2008. A Peer-to-Peer Electronic Cash System. Bitcoin. Available online at: https://bitcoin.org/bitcoin. pdf.
Naqvi, N., & Hussain, M. 2020. Evidence-based Blockchain: Findings from a Global Study of Blockchain Projects and Start-up Companies. The Journal of The British Blockchain Association: 16795. DOI: https://doi.org/10.31585/jbba-3-2-(8)2020
Office of the National Coordinator for Health Information Technology. 2015. Connecting Health and Care for the Nation, A Shared Nationwide Interoperability Roadmap, 1. Available online at: https://www.healthit.gov/sites/default/files/hie-interoperability/nationwide-interoperability-roadmap-final-version-1.0.pdf
Palombani, M. 2017. Blockchain & The Pharma Supply Chain - Beyond DSCSA Compliance, pharmaceuticalonline.com. Available online at: https://www.pharmaceuticalonline.com/doc/blockchain-the-pharma-supply-chain-beyond-dscsa-compliance-0001
Papi, E., Kuffour-Osei, D., Chen, Y., & McGregor, A. 2015. Use of Wearable Technology for Performance Assessment: a validation study. Medical Engineering and Physics, 37: 698-704.
Peng, L., Youn, C.H., Tang, W., Qiao, C. 2012. A Novel Approach to Optical Switching for Intra Datacenter Networking. Lightwave Technology, 230(2): 252-266.
Peterson, K., Deeduvanu, R., Kanjamala, P., & Boles, K. 2016. A Blockchain-Based Approach to Health Information Exchange Networks. Available online at: https://www.healthit.gov/sites/default/files/12-55-blockchain-based-approach-final.pdf
Reisman, M. 2017. EHRs: the challenge of making electronic data usable and interoperable. Pharmacy and Therapeutics, 42(9): 572.
Rangarajan, S., Liu, H., Wang, H., & Wang, C.L. 2015. Scalable Architecture for Personalized Healthcare Service Recommendation Using Big Data Lake. Service Research and Innovation: 65-79. DOI: https://doi.org/10.1007/978-3-319-76587-7_5
Scholl, M.A., Stine, K.M., Hash, J., Bowen, P., Johnson, L.A., Smith, C.D., & Steinberg, D.I. 2008. SP 800-66 Rev. 1. An introductory resource guide for implementing the health insurance portability and accountability act (HIPAA) security rule. Technical Report Gaithersburg, MD, USA: NIST. DOI: https://doi.org/10.6028/nist.sp.800-66r1
Schrauf, S. 2017. Digitizing the Supply Chain. Harvard Business Review, 10(17). Available online at: https://content.gihub.org/live/media/forms/upload/form_8f8eb6e2-e94f-4001-8a1d-e6bd1b28c766/cfc4fb5a-9695- 418c-8d38-59a1040d2275/ppphealth4all_compressed.pdf
Shen, B., Guo, J., & Yang, Y. 2019. Med Chain: Efficient healthcare data sharing via blockchain. Applied Sciences: 9. DOI: https://doi.org/10.3390/app9061207
Srinivasa, R.S. 2011. Ultra-Low Power Microcontrollers for Portable, Wearable, and Implantable Medical Electronics. MCU Development, Texas Instrument, Inc. Available online at: https://pdfs.semanticscholar.org/6da8/7a8faa359a61a68e856c347b8f52ac143a89.pdf
Stagnaro, C. 2019. White Paper: Innovative Blockchain Uses in Health Care. Available at https://www.freedassociates.com
Stanganelli, S. 2016. How Blockchain is Helping Genomics Research. Bio IT World. Available online at: http://www.bio-itworld.com/2016/5/4/how-blockchain-is-helping-genomics-research.aspx
Statista. Size of the blockchain technology market worldwide from 2018 to 2025. 2022. Available online at: https://www.statista.com/statistics/647231/worldwideblockchain-technologymarket-size
The Economist. 2015. The Trust Machine - The Promise of the Blockchain.
Tobin, A., & Reed, D. 2018. The Inevitable Rise of Self-Sovereign Identity. The Sovrin Foundation: Technical Report. Available online at: https://sovrin.org/wp-content/uploads/2017/06/The-Inevitable-Rise-of-Sel...
US Congress. 2015-2016. H.R.1806 - America COMPETES Reauthorization Act of 2015 114th Congress. Available online at: https://www.congress.gov/bill/114th-congress/house-bill/1806
U.S. Department of Health & Human Services. 2017. Individuals’ Right under HIPAA to Access their Health Information 45 CFR § 164.524, hhs.gov. Health Information Privacy. Available online at: https://www.hhs.gov/hipaa/for-professionals/privacy/guidance/access/
Valderas, J., Kotzeva, A., Espallargues, et al. 2008. The Impact of Measuring Patient-Reported Outcomes in Clinical Practice: a systematic review of the literature, Quality of Life Research, 17: 179- 93. DOI: https://doi.org/10.1007/s11136-007-9295-0
Vergel, D.D. 2016. Why we’re Building the Blockchain for Healthcare. Blogpost. Available online at: https://blog.gem.co/why-were-building-the-blockchain-for-healthcare-bda5c09870aa
Winton, R. 2016. Hollywood hospital pays $17,000 in bitcoin to hackers; FBI investigating. Los Angeles Times. Available online at: http://www.latimes.com/business/technology/la-me-ln-hollywood-hospital-bitcoin-20160217-story.html
Keywords: Blockchain Technology, Electronic Health Records, healthcare, Internet of Things